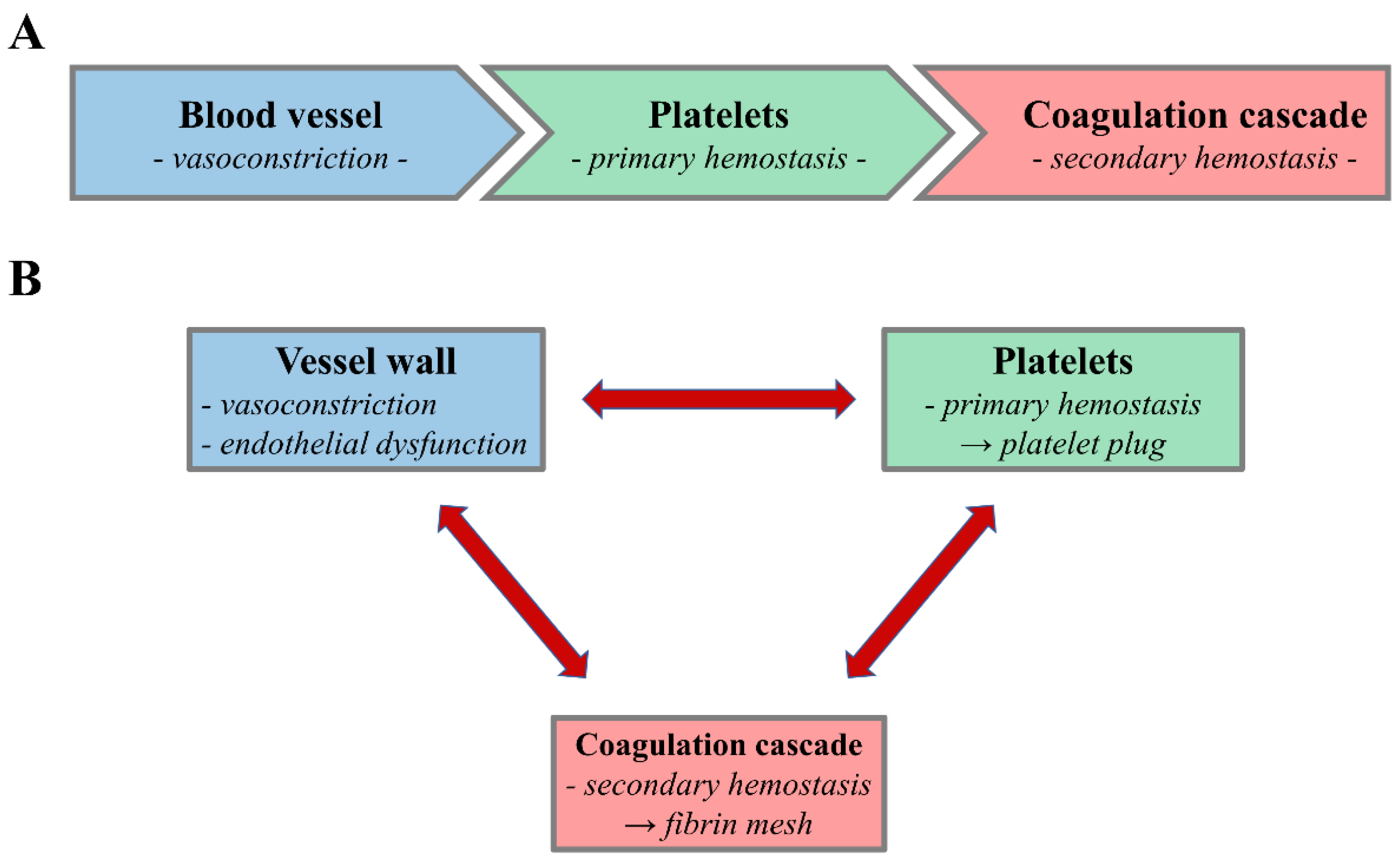
The blood clot pathway, also known as coagulation, is a critical process that prevents inordinate bleeding when a rakehell vessel is injured. This intricate cascade of events involves a series of protein, cognise as clotting factors, which act together to form a rake clot. Understanding the blood clotting pathway is crucial for perceive diverse medical conditions and treatments related to phlebotomize and clotting upset.
Understanding the Blood Clotting Pathway
The roue clabber pathway can be generally divide into two master pathways: the intrinsical pathway and the extrinsic tract. These tract meet to form a mutual tract that ultimately result to the formation of a rakehell coagulum.
The Intrinsic Pathway
The intrinsic pathway, also cognize as the contact energizing pathway, is initiated by the exposure of profligate to negatively supercharged surfaces, such as collagen or other subendothelial components. This pathway involves a serial of reactions that activate diverse coagulate factors. The key steps in the intrinsical footpath are as follows:
- Factor XII Activation: The process get with the activating of Factor XII (Hageman factor) when it comes into contact with negatively charged surfaces.
- Factor XI Activation: Actuate Factor XII then trip Factor XI.
- Factor IX Activation: Element XI activates Factor IX.
- Factor VIII Activation: Ingredient IX, in the front of Factor VIII, trip Factor X.
This episode of event leads to the activating of Factor X, which is a all-important step in the common pathway.
The Extrinsic Pathway
The extrinsic tract, also cognise as the tissue factor tract, is initiated by the exposure of blood to tissue element (TF), a protein launch in the subendothelial tissue. This footpath is typically activated when there is damage to the roue vas wall. The key measure in the extrinsic pathway are as follows:
- Tissue Factor Activation: Tissue ingredient attach to Factor VII, forming a complex that activates Factor X directly.
- Factor X Activation: The tissue factor-Factor VII complex also activate Factor IX, which can then trip Factor X through the intrinsic footpath.
Both the intrinsic and extrinsic pathway converge at the activating of Factor X, conduct to the common pathway.
The Common Pathway
The mutual footpath is the terminal point of the rake clot process, where the intrinsic and extrinsic pathways converge. This pathway regard the activating of Factor X, which guide to the shaping of a roue coagulum. The key steps in the common tract are as follow:
- Factor X Activation: Spark Factor X, in the presence of Factor V, calcium, and phospholipids, converts prothrombin (Factor II) to thrombin (Factor IIa).
- Thrombin Formation: Thrombin then convert fibrinogen (Factor I) to fibrin (Factor Ia), which organise a mesh-like construction that traps platelets and other rip cell, create a blood coagulum.
- Fibrin Stabilization: Factor XIII, actuate by thrombin, steady the fibrin meshing by cross-linking fibrin strands, create the coagulum more tolerant to abasement.
The mutual footpath is indispensable for the establishment of a stable rip coagulum that can efficaciously kibosh bleeding.
Regulation of the Blood Clotting Pathway
The rakehell clotting pathway is tightly influence to see that coagulum organise but when necessary and do not obstruct blood stream unnecessarily. Respective mechanisms are involved in the regulation of this footpath, including:
- Antithrombin: A protein that inhibits thrombin and other serine peptidase involved in the curdling footpath.
- Protein C and Protein S: These proteins demobilize Ingredient Va and VIIIa, preventing excessive clotting.
- Tissue Factor Pathway Inhibitor (TFPI): Inhibit the tissue factor-Factor VII composite, preventing uncontrolled activating of the extrinsic footpath.
These regulatory mechanisms secure that the blood clotting pathway operates expeditiously and safely.
Clinical Implications of the Blood Clotting Pathway
Understanding the blood clotting pathway is crucial for name and treat various aesculapian weather related to bleed and clotting disorders. Some of the key clinical deduction include:
- Hemophilia: A inherited disorder characterize by a inadequacy in clot factors, such as Factor VIII or Factor IX, leading to prolonged hemorrhage.
- Von Willebrand Disease: A disorder caused by a deficiency or disfunction of von Willebrand factor, which is crucial for platelet adherence and collecting.
- Thrombophilia: A stipulation that increases the risk of blood clots, often due to genetic mutations or acquired component.
- Deep Vein Thrombosis (DVT) and Pulmonic Embolism (PE): Conditions where blood clots organise in the deep veins of the leg or lung, severally, and can be life-threatening if not treat pronto.
Handling for these conditions ofttimes regard the use of anticoagulants, which inhibit the rip clotting pathway, or curdle component concentrate, which replace deficient factors.
Diagnostic Tests for Blood Clotting Disorders
Respective symptomatic test are uncommitted to assess the blood clabber pathway and identify potential disorders. Some of the most commonly put-upon examination include:
- Prothrombin Time (PT): Bill the clip it takes for blood to clot via the extrinsic tract.
- Activated Partial Thromboplastin Time (aPTT): Quantity the clip it takes for blood to coagulate via the intrinsical pathway.
- International Normalized Ratio (INR): A standardized step of PT, used to monitor anticoagulant therapy.
- Thrombin Time (TT): Measures the time it takes for thrombin to convert fibrinogen to fibrin.
- Factor Assays: Specific tests to quantify the activity of single clotting divisor.
These tests help healthcare providers diagnose and manage rakehell clotting disorders efficaciously.
Treatment Options for Blood Clotting Disorders
Handling for rakehell coagulation disorder depends on the specific condition and its asperity. Some mutual treatment options include:
- Anticoagulants: Medicament that inhibit the rip clotting pathway, such as coumadin, heparin, and unmediated oral anticoagulants (DOACs).
- Antiplatelet Agents: Medicine that prevent platelets from aggregating, such as empirin and clopidogrel.
- Clotting Factor Concentrate: Replacement therapy for patients with deficiencies in specific clotting factors, such as Factor VIII or Factor IX concentrates.
- Thrombolytics: Medicine that dissolve rip clot, such as tissue plasminogen activator (tPA).
These handling options are tailored to the individual needs of the patient and the specific roue clotting disorder.
📝 Note: Treatment decisions should always be make in reference with a healthcare provider, as the choice of medication and dose can vary based on individual patient factors.
Prevention of Blood Clotting Disorders
Preventing blood curdle disorders affect a combination of lifestyle qualifying and medical interference. Some key strategies include:
- Lifestyle Changes: Maintaining a salubrious weight, exercising regularly, and avoiding smoke can cut the risk of rakehell clots.
- Medicament: Decoagulant and antiplatelet agent may be prescribe to keep blood coagulum in high-risk individuals.
- Compaction Stockings: Wearing concretion stockings can help prevent deep vena thrombosis (DVT) by improve rake flow in the leg.
- Regular Check-ups: Veritable aesculapian check-ups can assist place and care risk divisor for blood clotting upset.
These preventive bill can importantly cut the risk of developing roue coagulation disorder and their associated complications.
Future Directions in Blood Clotting Research
The field of blood clotting research is continually develop, with new discoveries and furtherance being make regularly. Some of the key areas of focus include:
- Transmissible Studies: Identifying genetic mutations that contribute to blood curdle disorders and developing targeted therapy.
- Biomarkers: Discovering new biomarkers that can prefigure the peril of rip clots and reminder treatment effectiveness.
- Novel Therapeutics: Developing new medicine and therapies that can more effectively and safely manage blood clotting disorders.
- Personalized Medicine: Tailoring intervention plans to individual patient ground on their genetic constitution and specific jeopardy factors.
These advancements keep hope for better the diagnosis, intervention, and bar of blood coagulate disorders in the futurity.
to summarize, the blood clotting pathway is a complex and essential summons that play a crucial function in maintaining haemostasis and forbid excessive bleeding. Understanding the assorted components and mechanism of this pathway is critical for diagnosing and process blood coagulate upset. By stay inform about the modish research and advancements in this field, healthcare provider can offer better precaution and improve outcomes for patient with blood clotting disorders.
Related Terms:
- bleeding pathway
- intrinsical vs extrinsic clot pathway
- rakehell curdling pathway
- intrinsical curdling cascade
- clotting shower
- clotting pathway diagram